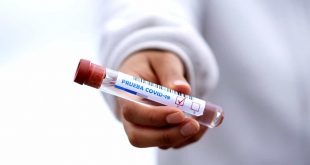
Barbara Lalonde holds a portrait of her parents. Her father, Arthur Harek, was a 95-year-old resident of Anson Place Care Centre in Hagersville, Ont., where he contracted COVID-19 and was rushed to hospital four times before his death on March 16.
Kate Dockeray/Globe and Mail
The first inkling that COVID-19 was inside Anson Place Care Centre, a seniors’ residence in Southwestern Ontario, came through a phone call in mid-March from the local public health unit: An animal handler who brought a parrot, a snake and a ferret to the home to entertain residents had been exposed to the virus at another seniors’ facility.
The privately owned home immediately went into lockdown, but lifted it three days later under the guidance of health officials. It would prove to be one of a series of fatal errors that allowed the virus to ravage the home in the rural community of Hagersville, near Hamilton, killing 27 of its 101 residents.
A Globe and Mail investigation found the outbreak resulted from failings at every level in the system designed to protect the frail elderly. The home, doctors at the local hospital, public health officials, provincial safety inspectors and Ontario’s top medical officer all missed early opportunities to prevent the spread of the virus.
Everyone from the management of the home to the Premier’s Office was slow to respond to cries for help from front-line health care workers, who were forced to ask both an Ontario Superior Court judge and the province’s quasi-judicial Labour Relations Board to intervene.
It was only on April 21 – nearly a month after the first outbreak at a nursing home in Ontario – that chief medical officer of health David Williams ordered local public health units to test everyone in long-term care homes for COVID-19, the respiratory disease caused by the novel coronavirus.
The Globe investigation is based on hundreds of pages of documents filed in Ontario Superior Court, internal corporate records, Ministry of Labour inspection reports and interviews with several individuals close to the situation at Anson Place. Among the findings:
- Management at Anson Place did not follow its own pandemic plan, but instead kept residents made ill by COVID-19 alongside the healthy, causing the virus to spread.
- Public health erroneously blamed the outbreak at Anson Place on those who attended a former resident’s funeral, while not doing enough to help the home contain the spread of the virus.
- The Ministry of Labour, which is responsible for ensuring that employers comply with workplace health and safety standards, has routinely inspected seniors’ homes by phone rather than in person during the pandemic. Of the 612 COVID-19-related inspections done since March 12, only 25 were in person, according to ministry figures provided to The Globe.
- Premier Doug Ford waited until mid-April to temporarily ban staff from working at more than one facility, even as the pandemic laid bare long-standing vulnerabilities in Canada’s nursing homes: low pay and a lack of full-time hours have forced staff to work at multiple homes.
Lisa Roth, executive director of Anson Place, said the home was guided in its handling of the outbreak by public health officials, and has worked closely with the local health unit and the provincial government to update its infection-control and outbreak-management policies as health experts continue to improve their understanding of the new virus.
“Due to COVID-19’s impact,” she said, “our team was faced with unprecedented challenges.”
The two-storey home has a retirement residence with 40 private rooms on the first floor and a long-term care unit on the second, with all but three of the 61 beds in shared wards. The long-term care unit was hit hardest, with 23 residents succumbing to the virus – a fatality rate of just less than 38 per cent. Four residents in the retirement unit died of the virus.
Anson Place is one of 11 for-profit homes in Ontario owned by Rykka Care Centres, a private Toronto-based company incorporated in 2006 by Ben Friedman and Sy Schachner, according to registration records. Mr. Friedman is the owner and chief executive of Saucham Holdings Ltd., a private real estate holding and development company (Neither he nor Mr. Schachner could be reached for comment). The vast majority of Rykka’s homes are older facilities where up to four residents share a room and one bathroom. All but two are classified as “C” homes, meaning they meet the provincial Ministry of Long-Term Care’s 1972 design standards.
Eight of Rykka’s homes have had outbreaks of COVID-19, according to the Long-Term Care Ministry. The courts ordered three of those homes where 112 residents died of the virus – Anson Place, Eatonville Care Centre in Toronto and Hawthorne Place Care Centre in North York – to provide nurses with access to N95 respirator masks and other personal protective equipment. The Ontario Labour Relations Board ordered the Ministry of Labour to conduct weekly, on-site inspections at Anson Place and Eatonville.
“Shame on people that it takes an order either from a court or from the Labour Relations Board to do the right thing to keep people safe,” said Sharleen Stewart, president of SEIU Healthcare, which represents 60,000 workers.
Ms. Lalonde stands next to her father’s old mailbox. She and 11 other family members tested positive for COVID-19 after her father died. ‘We’ve come to the assumption that Dad had it and that’s where we got it,’ she says.
Kate Dockeray/Globe and Mail
Arthur Harek, a 95-year-old retired farmer, was the first victim of the virus at Anson Place, but no one suspected it at the time.
In the days leading up to his death on March 16, Mr. Harek was rushed to the hospital in Hagersville four times, said his daughter, Barbara Lalonde. Doctors at West Haldimand General Hospital attributed his difficulty breathing, lethargy and a cough to his heart condition, and sent him back to the retirement home. The day before he died, she said, he was back in the hospital. “I felt his back and it was rattling like crazy.”
Shortly after, Ms. Lalonde, along with 11 members of her family, all tested positive for COVID-19.
“We’ve come to the assumption that dad had it and that’s where we got it,” she said.
Her family was shocked when the Haldimand-Norfolk Health Unit publicly blamed the outbreak at the long-term care facility on Mr. Harek’s funeral. “Staff have determined that a significant number of positive cases at Anson Place can be traced to attendance at a funeral,” a news release dated April 5 says.
Both Ms. Lalonde and the owner of the funeral home said that statement makes no sense. No one from Anson Place attended the funeral, Ms. Lalonde said, and no one from her family had any reason to return to the home after her father’s death.
Jill Thompson, the owner of Thompson-Mott Funeral Home, said 42 people, mostly family members, attended the service on March 20. No one from Mr. Harek’s family contracted the virus from her funeral home or any of its staff members, she said, adding that her own test results came back negative.
“I don’t understand why the medical officer said this,” Ms. Thompson said. “To say it started here just medically doesn’t make sense.”
Shanker Nesathurai, the medical officer of health for Haldimand-Norfolk, said in an e-mail to The Globe that the health unit does not comment on matters involving individual community members. “Assessments of this nature cannot be used to attribute blame to any individual,” he said.
Ms. Roth declined to comment on Mr. Harek’s death, citing privacy concerns.
A copy of an Anson Place employee’s Workplace Safety & Insurance Board report obtained by The Globe shows that a postmortem confirmed the first COVID-19 death at the home was March 16, the same day Mr. Harek died. It is not clear when the postmortem was done. A hospital official declined to comment, citing privacy concerns. Ms. Lalonde said no one told her family about the postmortem.
Two days after Mr. Harek’s death, a public health official warned Anson Place about a potential exposure to the coronavirus.
Rebecca Piironen, a personal support worker at Anson Place who answered the phone call, said the official asked if an animal trainer had visited the home. When she said the trainer had entertained residents in the home’s retirement unit on March 6, she said, the official “let us know the handler had come in contact with COVID-19 at another nursing home.”
The next thing she knew, retirement residents on the first floor were confined to their rooms for three days, and staff on their unit were wearing full PPE.
But Ms. Piironen and other front-line staff who work on the long-term care unit on the second floor were not given PPE, she said, creating fears the home wasn’t taking proper precautions to protect workers and residents. Staff on the retirement and long-term care units share the same lunchroom and change room.
Another employee who asked not to be named out of concerns for her job said staff repeatedly asked the home’s executive director, Ms. Roth, why the unit had been locked down. “She just kept saying, ‘Don’t worry. It’s not COVID related,’” the employee said. “She kept telling us that over and over again.”
Anson Place ceased “isolation protocols” after receiving direction from public health, Ms. Roth said in an e-mail to The Globe. The home relies on the health unit for advice during respiratory outbreaks, she said, and officials never clarified whether the potential exposure in the home from the animal handler was COVID-19.
Dr. Nesathurai said in the e-mail to The Globe that his health unit advised Anson Place on the most appropriate approach to manage the exposure, while protecting a community member’s confidential information. “As such,” he said, “health unit practice related to exposures of this nature does not include disclosing the specific disease.” With regards to ending the isolation protocols, he said the decision was made based on the “course of the exposure.”
Earlier in the pandemic, he said, patients were tested only if they had symptoms of the disease, adding that there can be a long time between exposure and laboratory confirmation of COVID-19.
The animal handler declined to talk to The Globe. His lawyer said no one who works for the handler had any symptoms of the virus on March 6, but would not say whether her client eventually tested positive for the virus.
Ruby McCarroll, 95, died of COVID-19 in hospital but was believed to have contracted the virus at Anson Place.
Handout
It would be March 27 before Anson officially declared an outbreak. That same day, Mr. Harek’s close friend in the retirement unit, Ruby McCarroll, tested positive for COVID-19.
Her son, Mike McCarroll, said his mother, a 95-year-old retired teacher, was mentally sharp in early February when she celebrated her grandson’s birthday at a Red Lobster restaurant. But on March 23, she was hospitalized with a low-grade fever. She died on March 30.
“To figure out where the virus came from, the medical officer [of health] should have talked to people,” said Mr. McCarroll, the lead plaintiff in a proposed class-action lawsuit against Anson Place. “He never talked to me.”
A heart hangs on Anson Place’s fence in April. Few of the beds here are in private rooms where residents could isolate from others; most are in wards with two or four beds.
Frank Gunn/The Canadian Press
By the end of March, the virus had spread quickly from the retirement residence on the first floor to the long-term care unit on the second floor. Staff were also getting sick, including Ms. Roth. She tested positive on March 31, according to her affidavit filed in court.
When staff at Anson Place complained to the Ontario Ministry of Labour about unsafe working conditions, including a lack of PPE, Shelly Speir, an inspector at the ministry, followed up by telephone instead of visiting the home.
Anson Place breezed through the first review on March 30, without a single order issued against it, according to a copy of the inspection report. In the second review on April 8, also by phone, the inspector told Anson Place to make face masks available for night staff, the report says.
On April 24, the Ontario Labour Relations Board ordered the Ministry of Labour to conduct weekly in-person inspections at Anson Place for the next two months. Three days later, Ms. Speir showed up at the home to see things for herself. She found plenty of problems that day.
In her written report obtained by The Globe, Ms. Speir cites Anson Place for nine violations of provincial laws designed to protect workers from hazards on the job. Among them: The person screening staff and visitors at the front door was not wearing protective eye goggles, and had to be reminded three times to take Ms. Speir’s temperature; boxes of surgical masks were left open in a hallway, exposing them to contamination; workers who left the home during breaks returned wearing the same potentially contaminated face masks. By that time, 27 of the 101 residents had died and all but 29 of the survivors had tested positive for COVID-19. The home accounts for all but four deaths from the virus in the rural community.
Ms. Speir declined to comment when reached by The Globe. A spokesperson at the Ministry of Labour said it halted in-person inspections during the pandemic to help stop the virus from spreading in long-term care homes. Many complaints have revolved around PPE, the spokesperson said. “Often, these concerns can be dealt with remotely to the satisfaction of both the worker and employer without orders being issued.”
Workers walk out to form a shield as a body is removed from Anson Place on April 22.
Frank Gunn/The Canadian Press
The Ontario Nurses Association (ONA) accuses three of Rykka’s homes in court documents of keeping residents made ill by COVID-19 with the healthy, causing the virus to spread, and of “severely” limiting staff members’ access to PPE, including N95 respirator masks.
Ian Dick, a lawyer for Rykka, argued in court on April 22 that Anson Place is exempt from a provincial directive requiring sick residents to be segregated from healthy ones because of its small size. The long-term care unit has 15 rooms with two beds and seven with four beds, according to Rykka’s service-accountability agreement with the province.
The directive from Ontario’s Chief Medical Officer says, “In smaller long-term care homes or in homes where it is not possible to maintain physical distancing of staff or residents from each other, all residents or staff should be managed as if they are potentially infected.” Staff are required to wear surgical masks and other PPE.
Anson Place, it turns out, did not follow its own pandemic plan. A copy of the document dated May 14, 2018, prepared by Responsive Management Inc., Rykka’s operating partner, says “residents will be segregated in specific areas in order to separate influenza and non-influenza residents to minimize the potential spread of organisms.” Instead, Anson Place closed a cloth curtain between ward beds to try to stop transmission of the virus. It also assumed all residents had tested positive for COVID-19, meaning they were kept in their rooms at all times, including for meals.
An Ontario Superior Court judge ordered the Rykka homes to make PPE available to nurses and to isolate residents sick with the disease during the crisis.
No one at Anson Place has died since April 22, and only 22 residents remain ill with the virus, prompting Ms. Roth to say she believes the home is “turning the corner.”
Ms. Piironen, the personal support worker who has been off work sick since early April with many symptoms of the virus but has tested negative, says she feels betrayed by everyone responsible for safe-guarding the home. “They didn’t protect us. They didn’t protect the residents. They didn’t protect our community,” she said.
With a report from Rick Cash
Overview: Ontario’s worst-hit seniors’ homes
Our Morning Update and Evening Update newsletters are written by Globe editors, giving you a concise summary of the day’s most important headlines. Sign up today.
 The Argus Report Read about it!
The Argus Report Read about it!