Getty
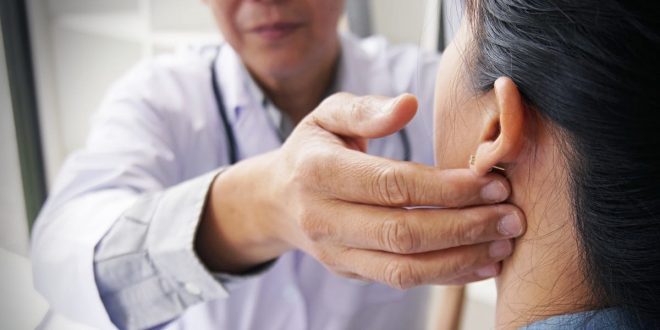
- The CDC recently added four new COVID-19 symptoms — fatigue, diarrhea, congestion or runny nose, and nausea or vomiting — to its official list.
- Fever and cough are the most common symptoms of COVID-19.
- Shortness of breath, which is also common, is often the most dangerous.
- Smaller groups of patients report additional symptoms like muscle pain, sore throat, and loss of taste or smell.
- Visit Business Insider’s homepage for more stories.
When the novel coronavirus was first identified in China, patients seemed to develop at least one of three symptoms: fever, a dry cough, and shortness of breath. The data was skewed, however, by the fact that most patients being tested for the virus had severe cases that required hospitalization.
As the virus grew to pandemic proportions, doctors have observed many additional symptoms. Some patients report muscle aches, while others develop purple, swollen toes that appear frostbitten. The US Centers for Disease Control and Prevention has been updating its official list of COVID-19 symptoms since the pandemic began, adding more as research grows more robust. Most recently, the agency added fatigue, diarrhea, congestion or runny nose, and nausea or vomiting to the list.
Scientists have also discovered that the virus can infect the heart, kidneys, liver, and intestines. This can lead to additional complications like heart damage or acute kidney failure.
Here’s a rundown of how each symptom manifests among typical patients.
The CDC now lists 11 symptoms associated with COVID-19.
U.S. Navy/Chief Mass Communication Specialist Barry Riley/Handout via Reuters
These symptoms usually appear two days to two weeks after exposure to the virus, according to the CDC.
- Fever or chills
- Cough
- Shortness of breath or difficulty breathing
- Fatigue
- Muscle or body aches
- Headache
- New loss of taste or smell
- Sore throat
- Congestion or runny nose
- Nausea or vomiting
- Diarrhea
Fever is the most common symptom.
AP Photo/Vincent Thian
A February report from the World Health Organization found that out of nearly 56,000 laboratory-confirmed cases studied in China, about 88% of patients developed a fever.
The second-most common is a dry cough, though COVID-19 patients can also develop a wet cough.
Crystal Cox/Business Insider
The WHO report found that 68% of patients developed a dry cough. But a study in Wenzhou, China found that about one-third of patients (13 of 53) developed a wet cough.
Fatigue can be more common than difficulty breathing, according to the WHO.
Crystal Cox/Business Insider
The WHO report found that 38% of patients developed fatigue as a result of COVID-19.
The Wuhan study found the symptom to be even more common: 70% of those patients developed fatigue.
Around 20% of patients develop shortness of breath, which doctors recognize as one of the most concerning symptoms.
Reuters/Stephane Mahe
Difficulty breathing can be an early sign of pneumonia or acute respiratory distress syndrome (ARDS), an often fatal illness that may require intubation.
A study of 138 hospitalized patients in Wuhan, China, found that 31% of all patients had difficulty breathing. Among ICU patients, that number was 64%.
“I would of course always ask about shortness of breath before anything, because that’s somebody who has to be immediately helped,” Megan Coffee, an infectious-disease clinician in New York City, previously told Business Insider.
Shortness of breath typically presents eight to 10 days into the course of the illness, she said. But not every patient with shortness of breath needs to go to the hospital.
“What I tell people is: If you’re feeling short of breath and it’s hard to walk across the room, walk up a flight of stairs, speak in full sentences — those are always signs that you have more severe shortness of breath,” Coffee said.
Patients have reported additional respiratory symptoms like wheezing and chest pain.
Crystal Cox/Business Insider
Nearly 23% of patients in the Wenzhou study experienced wheezing.
The CDC lists “persistent pain or pressure in the chest” as an emergency warning sign, meaning people with the symptom should seek medical attention right away.
Bluish skin or lips are not common, but they’re signs of a serious infection, since they signal a lack of oxygen in the blood.
Zay Nyi Nyi/Shutterstock
Doctors look for oxygen levels between 95% and 100% for healthy patients. A patient’s skin typically turns blue (what’s known as “cyanosis”) when their oxygen levels are below 90% — a sign of a clinical emergency, according to the WHO.
In the case of COVID-19, blue lips or skin can signal the presence of pneumonia or ARDS. The CDC lists this symptom as one of its emergency warning signs.
Muscle pain developed among 15% of patients in the WHO report.
Crystal Cox/Business Insider
The report put muscle pain (clinically known as “myalgia”) in the same category as joint pain (or “arthralgia”). Both are commonly associated with viral infections.
In the Wuhan study, 35% of patients developed muscle pain or aches, though only 10% of patients in the Wenzhou study had the same symptoms.
Sore throat and headache seem to affect the same number of patients: around 14%, according to the WHO.
Lee Charlie/Shutterstock
Since both are considered mild symptoms, patients with a headache or sore throat may be less likely to go to the hospital or seek out a test, so data about the prevalence of those symptoms could be skewed.
The Wuhan study, for instance, found that around 17% of patients developed a sore throat, while less than 7% developed a headache.
The CDC includes chills on its list of symptoms.
Crystal Cox/Business Insider
Around 11% of Chinese patients involved in the WHO report developed chills.
Both chills and shivering are the product of muscles contracting and relaxing inside the body. Like a fever, they help raise a person’s body temperature to fight off infection.
An episode of shaking and chills accompanied by a fever is known as a “rigor.” It can also cause profuse sweating.
Loss of taste or smell can appear on its own or alongside other symptoms.
Reuters/Nicky Loh
The CDC lists the loss of taste and smell as a COVID-19 symptom, but it’s still unclear how common it is.
An April study of more than 200 hospitalized coronavirus patients in Wuhan, China, found that only 5% had loss of taste and smell. But another study of 50 coronavirus patients the same month found that 98% had at least some “smell dysfunction.”
The reality is likely somewhere in the middle: A May review found that around 53% of coronavirus patients had smell dysfunction. A Spanish case study also found that nearly 40% of patients with COVID-19 developed smell and/or taste disorders, compared to just 12% of patients with the flu.
The virus can cause blood clots to form, which leads to a host of health complications.
A Dutch study of 184 coronavirus patients in the ICU found that nearly one-third of patients had blood clots.
Scientists still aren’t sure why. It’s possible that the virus attacks blood vessels directly, but it could also induce a strong inflammatory response that damages those vessels. Since the coronavirus is a respiratory virus, it might also damage blood vessels by depleting oxygen levels in the blood.
“The number of clotting problems I’m seeing in the ICU, all related to COVID-19, is unprecedented,” Dr. Jeffrey Laurence, a hematologist at Weill Cornell Medicine in New York City, told CNN in April. “Blood clotting problems appear to be widespread in severe COVID.”
Blood clots can also lead to kidney or heart damage.
Radu Sigheti/Reuters
Blood clots can reduce blood flow to the kidneys and heart, resulting in damage to both organs. It’s also possible that the coronavirus attacks these organs directly, since both the heart and kidneys are rich in ACE2 receptors.
In general, coronavirus patients with preexisting health issues are at higher risk of heart damage or kidney failure.
A study of 416 hospitalized patients in Wuhan found that patients with a heart injury — around 20% — were typically older and had underlying issues like hypertension.
Hospitals have also recorded gastrointestinal symptoms like diarrhea, nausea, or vomiting. They may be an early sign of the virus.
PATRICK HERTZOG/AFP via Getty Images
Just 5% of coronavirus patients in the WHO report developed nausea or vomiting, and another 4% developed diarrhea.
But a March study of 204 hospitalized patients in China’s Hubei province found that more than 50% of patients reported digestive symptoms like lack of appetite, diarrhea, vomiting, or abdominal pain.
Nearly 13% of patients in the Wenzhou study had diarrhea. Similarly, the study of Wuhan patients found that 10% had diarrhea and nausea, while less than 4% experienced vomiting. The study found that diarrhea and nausea typically appeared one to two days before fever and difficulty breathing.
A recent Nature study found that the coronavirus actively replicates in the intestines, suggesting that the intestinal tract “might be a transmission route” for the virus.
Nasal congestion isn’t a common symptom, according to the WHO, but some patients have it.
Hyungwon Kang/Reuters
Nearly 5% of patients in the WHO report developed nasal congestion compared to around 7% in the Wenzhou study.
Features
coronavirus
Symptoms
Health
 The Argus Report Read about it!
The Argus Report Read about it!